If you work in post-acute or long-term care, you’ve probably noticed a significant shift in skilled nursing facilities (SNFs) — and it’s not something they’ve chosen. The landscape is changing, and it’s changing fast.
Across the country, SNFs are now caring for residents who just a few years ago would have stayed longer in the hospital. The stakes are higher: more complex respiratory cases, residents who need significantly more help with mobility, and greater care needs across the board. This trend has a name — acuity creep — and it’s redefining post-acute and long-term care as we know it.
The Infrastructure Gap Driving Acuity Creep in Skilled Nursing Facilities
Acuity creep means resident needs are ramping up much faster than buildings, equipment, or workflows can keep pace. With hospitals discharging patients sicker and sooner — all to meet value-based benchmarks — SNFs are left managing the fallout.
Here’s what’s really happening: today’s skilled nursing facility looks and acts more like a sub-acute hospital, but without the design or resources to match.
Facilities are now caring for residents who need:
- Continuous or intermittent oxygen therapy
- Upright positioning for breathing support
- Early, intensive help with mobility
- Regular repositioning to prevent pressure injuries
But most facilities, beds, and workflows were designed for a much lower-acuity population.
The Head-of-Bed Dilemma in SNFs: Breathing or Skin?
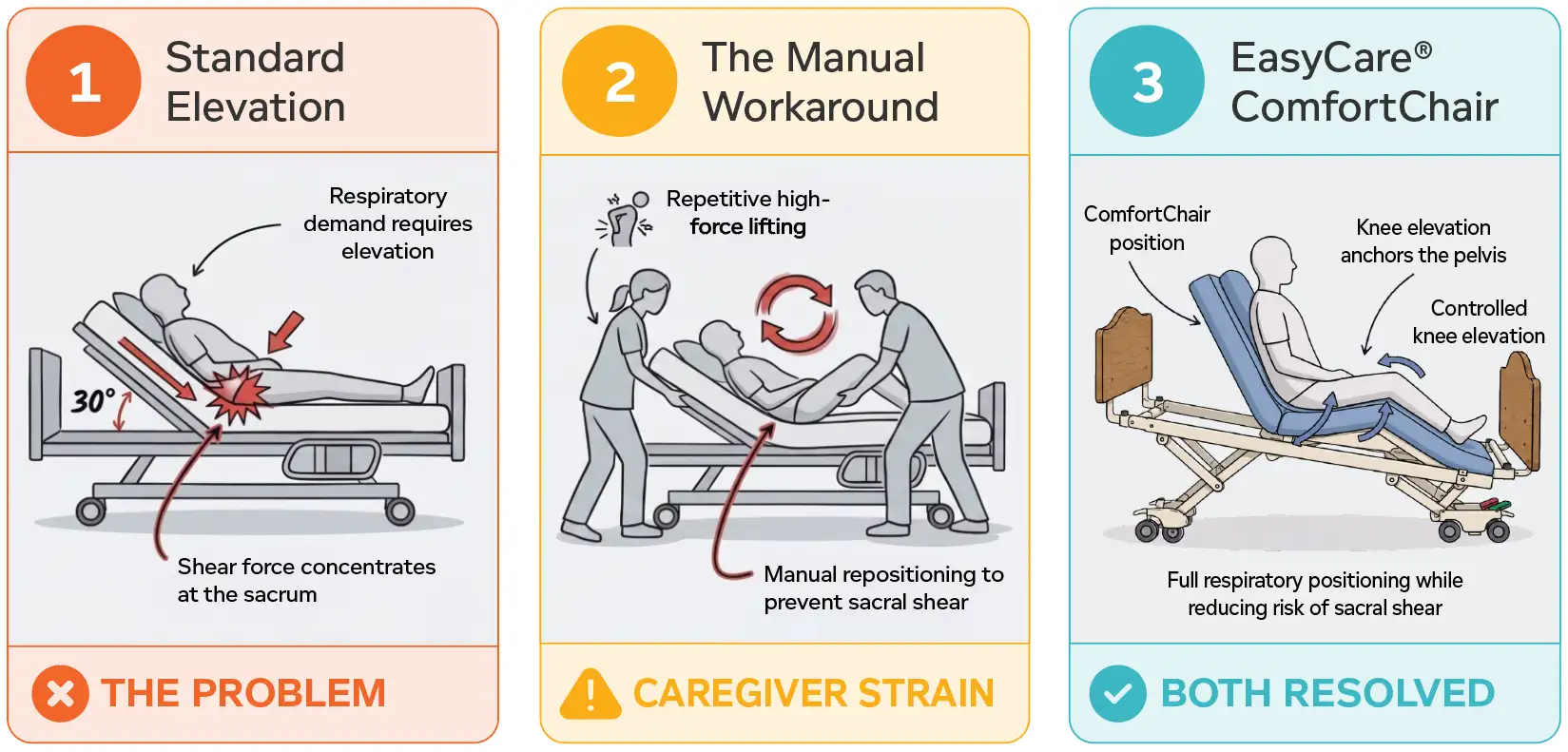
You can see acuity creep in action at the bedside. High-acuity respiratory residents often need their head elevated well above 30 degrees for proper breathing, aspiration prevention, or enteral feeding. But traditional wound care guidance warns against this, because elevation can cause sacral shear and tissue damage.
Nurses and aides are left with a difficult call:
- Raise the bed and support the lungs
- Or keep it flat and protect the skin
This isn’t about poor nursing — it’s about an infrastructure gap. Without beds that properly articulate, surfaces that reduce shear, and repositioning tools that reduce physical demand on staff, every increase in acuity creates more risk for both residents and caregivers.
Mobility Challenges in Post-Acute Care: The New Normal
Acuity creep also means more admissions with decreased mobility and slower recovery. More residents need:
- Help with sitting up or moving to the edge of the bed
- Frequent repositioning and turning
- Safe transfers, even when they can’t bear much weight
When facilities rely on staff to manually move residents through every one of these tasks, it leads to injuries, exhaustion, and burnout — especially against the backdrop of today’s staffing pressures. In a sub-acute environment, mobility support needs to be built into the system, not left to improvisation at every shift.
Outdated Infrastructure: The Real Driver of Acuity Creep Risk
Too many providers approach acuity creep as a staffing or training problem. It isn’t. You cannot safely care for complex respiratory or mobility-limited residents using:
- Beds that don’t keep the pelvis stable when the head is raised
- Surfaces that generate shear at higher angles
- Manual handling strategies that put the full physical burden on caregiving staff
Bed, surface and mobility equipment mismatch leads to falls, pressure injuries, staff injuries, and readmissions — and acuity creep reveals those infrastructure weaknesses faster than any census increase ever could.
How Skilled Nursing Facilities Can Tackle Acuity Creep
Meeting the needs of today’s post-acute population requires a shift in mindset — from custodial care to sub-acute intervention. Facilities that make this shift prioritize four things:
1. Beds Built for Active Care
Beds that support frequent movement and upright positioning — without adding shear or instability — are no longer optional. The ability to elevate for respiratory support while keeping the pelvis anchored is the difference between a tool that creates clinical tradeoffs and one that resolves them.
2. Support Surfaces That Perform When Elevated
Support surfaces need to perform not just when flat, but also when the head of the bed is raised for breathing, feeding, or swallowing therapy. A surface that can’t maintain its protective properties at higher angles is only doing part of its job.
3. Mobility as a Routine, Not a One-Time Event
Safe resident handling and mobility equipment should make movement safe and expected, not physically demanding and rare. When the equipment does more of the work, caregivers can focus on the resident rather than managing the physical load of the task itself.
4. Workflows That Reduce the Physical Load
The safest care environments are those where the facility’s systems and equipment carry as much of the physical burden as possible. When workflows are designed around that principle, staff fatigue decreases, injury risk drops, and consistency of care improves across every shift.
Bottom Line: Acuity Creep Is an Infrastructure Challenge
Acuity creep isn’t going away. If anything, it’s accelerating as hospitals continue to prioritize their own outcomes and financial performance.
The facilities that thrive will be those that face the facts: you cannot deliver sub-acute care in a building designed for long-term custodial care. The future of post-acute and long-term care belongs to those who close the gap — by updating infrastructure, equipment, and workflows to match what today’s residents actually need.
Because acuity doesn’t wait for your next renovation.
References
American Health Care Association (AHCA). (2024). Skilled nursing facility occupancy and acuity trends. Washington, DC: AHCA.
National Pressure Injury Advisory Panel (NPIAP). (2019). Prevention and treatment of pressure injuries: Clinical practice guideline. npiap.com
Centers for Medicare & Medicaid Services (CMS). (2024). Nursing facility staffing and quality measures. cms.gov
Waters, T.R., et al. (2011). Safe patient handling training for schools of nursing. National Institute for Occupational Safety and Health (NIOSH). cdc.gov/niosh
Author Bio
Michael Fragala, PhD, MBA, RN, WCC, CSPHP, AMS, is VP of Clinical Solutions at Joerns Healthcare and a nationally recognized expert in safe patient handling, wound care, and post-acute care operations. With decades of clinical and operational experience in skilled nursing and long-term care environments, Mike authors Joerns’ clinical thought leadership program and serves as a subject matter expert on acuity management, pressure injury prevention, and caregiver safety.
