In the high-pressure environment of Long-Term and Post-Acute Care (LTPAC), caregiver safety is directly tied to operational success. To reduce caregiver injuries in LTPAC, facilities must address one of the most persistent and preventable challenges in healthcare today: musculoskeletal disorders (MSDs).
With the average cost of a caregiver back injury hovering around $24,000 per incident (before accounting for indirect costs like replacement staffing and training), facilities can no longer view equipment as disparate purchases. To secure a sustainable Return on Investment (ROI), we must shift the conversation toward integrated care ecosystems—solutions engineered to minimize physical strain on caregivers, not contribute to it.
Reduce Caregiver Injuries in LTPAC With a System-Level Approach
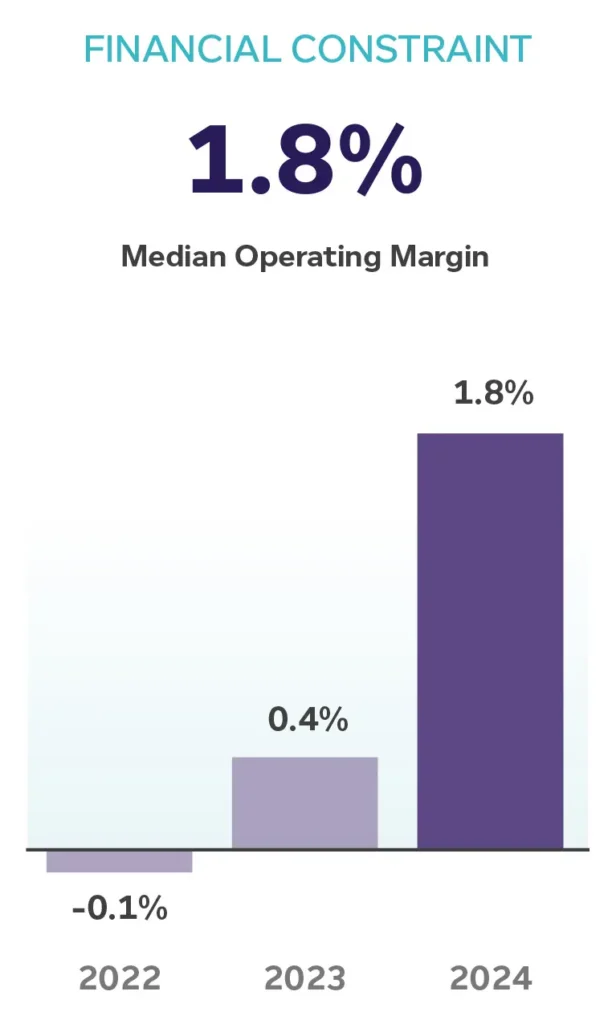
The Escalating Challenge: Acuity, Staffing, and Compatibility
The risk to caregivers is compounded by three specific industry trends. It is not merely that the work is hard; it is that the variables involved in resident handling are becoming more complex.
- Rising Resident Acuity and Bariatric Needs: As LTPAC facilities accept residents with higher acuity levels and higher BMIs, the physical demands on caregivers increase. Standard transfers now require significant force, heightening the risk of injury—one of the leading causes of lost workdays in healthcare, according to the CDC.
- The Staffing Crisis: Chronic shortages mean fewer hands on deck. Caregivers are often rushing to answer call lights or attempting transfers with suboptimal assistance because help isn’t immediately available. Fatigue leads to poor body mechanics, which can result in injury.
- Workflow Friction: An often-overlooked risk factor is the resistance caregivers face during transfers. This implies both the physical resistance of a lift hitting a damaged frame and the operational resistance of complex controls. When tools fight the workflow, safety protocols are the first thing to break down.
The Solution: Integrated, Ergonomic Design
To break the cycle of injury and turnover, facilities need an integrated approach to capital equipment that leverages solutions specifically engineered for seamless interoperability.
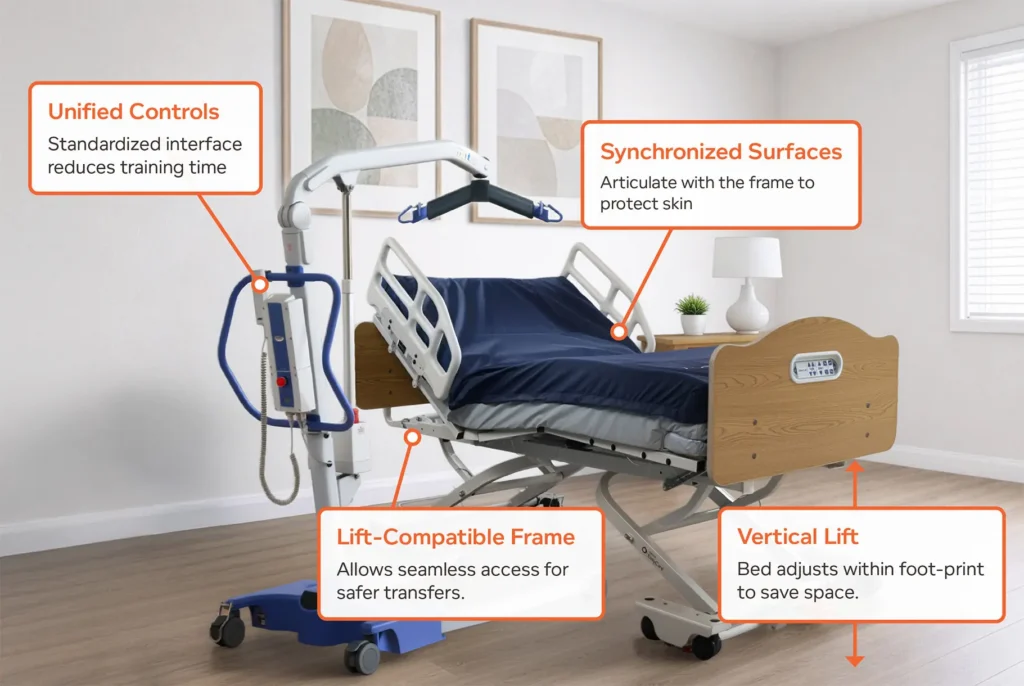
Joerns’ integrated care solutions address the root causes of caregiver strain through three core design principles:
1. Ergonomics that match Biomechanics
Lifts must do more than just hoist; they must mimic natural movement. Advanced ergonomic lifts support safer transfers by maintaining the resident’s center of gravity, reducing the push/pull force required by the caregiver. This transforms a high-exertion task into a guided, mechanical process.
2. Lift-Compatible Frames for Seamless Access
Resistance leads to strain. Unlike standard frames that may obstruct equipment, Joerns beds feature lift-compatible frames engineered for seamless access. By focusing on structural durability, these frames maintain their integrity against daily wear and tear. This ensures the under-bed area remains open and accessible, allowing lifts to slide underneath without obstruction and eliminating the “wrestling” often required to position a lift around a damaged frame.
3. Reduced cognitive strain via Unified Controls
In a high-stress clinical environment, complexity is a safety hazard. Unified, intuitive controls across equipment fleets reduce the cognitive strain on staff. When controls are simple and standardized, caregivers are more likely to take the necessary safety steps—such as raising the bed to the proper working height—rather than rushing through a transfer. This shortens training time, increases compliance with safety protocols, and boosts confidence.
The Outcome: ROI Beyond the Balance Sheet
When facilities transition from disjointed equipment to standardized, intuitive solutions, the impact is measurable across the organization.
- Financial ROI: Drastic reduction in workers’ compensation claims and the associated costs of temporary staffing agencies.
- Operational ROI: Greater confidence during transfers leads to more consistent care delivery and efficient workflows.
- Human ROI: When caregivers feel physically safe and supported by their equipment, morale improves. In an industry fighting for talent, providing the best tools is a powerful retention strategy.
Conclusion
Protecting your workforce is not just a clinical imperative; it is a financial necessity. By closing the gap between equipment and workflow, you can build a safer environment for your staff and a higher quality of life for your residents.